In the pursuit of speed, athletes and coaches often focus on acceleration, sprint mechanics, and max velocity. While these are essential components, one of the most overlooked and undertrained aspects of speed is deceleration—the ability to absorb, control, and redirect force efficiently.
Deceleration isn’t the opposite of speed. It’s the control system that allows speed to be useful in sport. Without it, athletes lack the ability to stop, change direction, or safely recover from explosive efforts.
Why Deceleration Matters
Most injuries—especially non-contact injuries—occur during deceleration or transition phases, not max effort sprints. ACL tears, hamstring strains, and ankle sprains are commonly linked to poor braking mechanics.
Key roles of deceleration include:
- Eccentric strength control to slow the body safely
- Joint stability during high-speed transitions
- Movement precision for change of direction and agility
- Energy absorption to reduce impact on tendons and ligaments
An athlete who cannot decelerate properly is at a higher risk for injury and performance breakdown, regardless of how fast they can run.
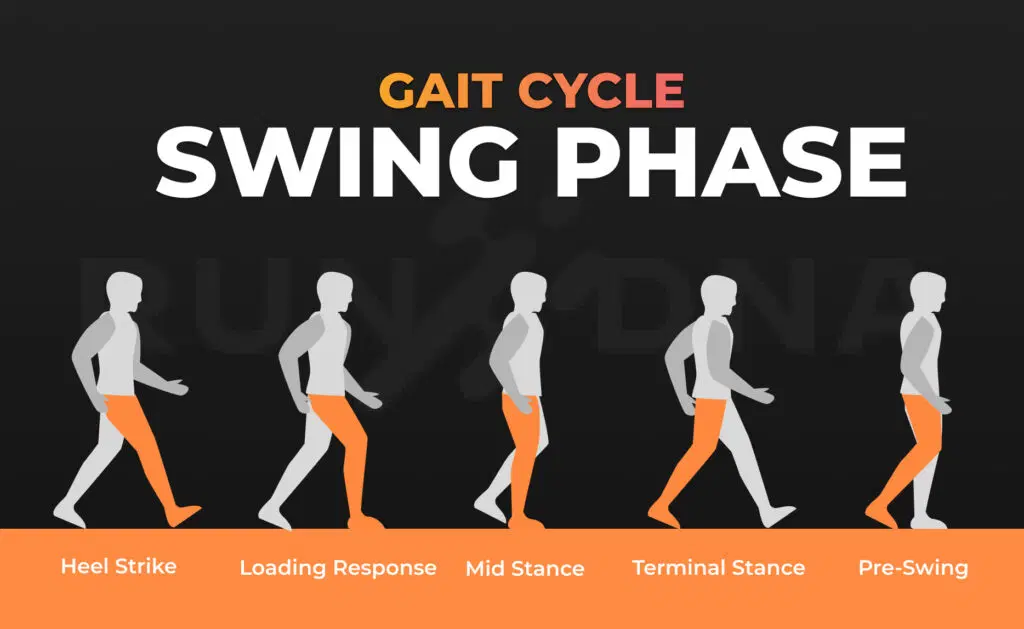
What Deceleration Looks Like
Effective deceleration involves:
- Proper body angles (hip and knee flexion)
- Center of mass control
- Strong eccentric strength in the posterior chain
- Ground contact mechanics that support rapid stopping without collapse or stiffness
Poor deceleration often appears as:
- Upright posture with little bend
- Excessive forward momentum
- Loud or unstable foot strikes
- Inability to re-accelerate quickly or efficiently
Training for Deceleration
To improve deceleration, athletes must train:
- Eccentric strength (e.g., Nordic hamstring curls, slow tempo lunges)
- Landing mechanics (e.g., drop landings, single-leg hops with stick)
- Reactive drills that require quick stops or redirects
- Controlled deceleration from sprints, shuffles, and bounds
Training should include both pre-planned and reactive deceleration tasks to simulate real-game movement demands.
The Takeaway
True speed isn’t just about how fast you go—it’s about how well you stop. Deceleration is the braking system of performance. Without it, acceleration becomes dangerous. With it, athletes gain control, efficiency, and resilience.
Speed training without deceleration is incomplete.
Teach it. Train it. Measure it.
Sources
- Hewett, T. E., Ford, K. R., & Myer, G. D. (2006). Anterior cruciate ligament injuries in female athletes: Part 1. The American Journal of Sports Medicine, 34(2), 299–311.
- Duhig, S. J., et al. (2016). Effect of deceleration load on muscle damage in professional Australian footballers. International Journal of Sports Physiology and Performance, 11(8), 1059–1065.
- Spiteri, T., et al. (2015). Contribution of strength characteristics to change of direction and agility performance in female basketball athletes. Journal of Strength and Conditioning Research, 29(8), 2205–2213.
- Harper, D. J., & Kiely, J. (2018). Damaging nature of decelerations: Do we adequately prepare players? BMJ Open Sport & Exercise Medicine, 4(1), e000379.